Prevalence and impact of diabetes in hospitalized COVID-19 patients: A systematic review and meta-analysis
住院新型冠状病毒肺炎患者糖尿病患病率及其影响的系统回顾和meta分析
Funding information: NSW Ministry of Health, Grant/Award Number: NSW Brain Clot Bank [2019-2022]
Abstract
enBackground
Diabetes is a cardiometabolic comorbidity that may predispose COVID-19 patients to worse clinical outcomes. This study sought to determine the prevalence of diabetes in hospitalized COVID-19 patients and investigate the association of diabetes severe COVID-19, rate of acute respiratory distress syndrome (ARDS), mortality, and need for mechanical ventilation by performing a systematic review and meta-analysis.
Methods
Individual studies were selected using a defined search strategy, including results up until July 2021 from PubMed, Embase, and Cochrane Central Register of Controlled Trials. A random-effects meta-analysis was performed to estimate the proportions and level of association of diabetes with clinical outcomes in hospitalized COVID-19 patients. Forest plots were generated to retrieve the odds ratios (OR), and the quality and risk assessment was performed for all studies included in the meta-analysis.
Results
The total number of patients included in this study was 10 648, of whom 3112 had diabetes (29.23%). The overall pooled estimate of prevalence of diabetes in the meta-analysis cohort was 31% (95% CI, 0.25-0.38; z = 16.09, P < .0001). Diabetes significantly increased the odds of severe COVID-19 (OR 3.39; 95% CI, 2.14-5.37; P < .0001), ARDS (OR 2.55; 95% CI, 1.74-3.75; P = <.0001), in-hospital mortality (OR 2.44; 95% CI, 1.93-3.09; P < .0001), and mechanical ventilation (OR 3.03; 95% CI, 2.17-4.22; P < .0001).
Conclusions
Our meta-analysis demonstrates that diabetes is significantly associated with increased odds of severe COVID-19, increased ARDS rate, mortality, and need for mechanical ventilation in hospitalized patients. We also estimated an overall pooled prevalence of diabetes of 31% in hospitalized COVID-19 patients.
摘要
zh背景
糖尿病是心脏代谢性伴随疾病, 可能使新型冠状病毒肺炎患者的临床结局更差。本研究旨在通过系统回顾和meta分析, 确定住院新型冠状病毒肺炎患者中糖尿病的患病率, 并调查糖尿病与严重新型冠状病毒肺炎疾病, 急性呼吸窘迫综合征(ARDS)发生率, 死亡率和机械通气需求之间的关系。
方法
从PubMed, Embase和Cochrane Central Register of Control Trials中选择个别研究, 采用定义的搜索策略, 包括截至2021年7月的结果。对住院的新型冠状病毒肺炎患者进行随机效应meta分析, 以评估糖尿病与临床结果的比例和水平。生成森林图以检索优势比, 并对meta分析中包括的所有研究进行质量和风险评估。
结果
本研究共纳入患者10648例, 其中糖尿病患者3112例(29.23%)。Meta分析队列中糖尿病总体合并估计的患病率为31%(95% CI 0.25-0.38, z=16.09 p<0.0001)。糖尿病显著增加严重新型冠状病毒肺炎严重程度(OR 3.39, 95% CI 2.14~5.37, p<0.0001), 急性呼吸窘迫综合征(OR 2.55, 95% CI 1.74~3.75, p=<0.0001), 住院死亡率(OR 2.44, 95% CI 1.93~3.09, p<0.0001)和机械通气(OR 3.03, 95%CI 2.17~4.22, p<0.0001)。
结论
我们的meta分析显示糖尿病与住院患者严重新型冠状病毒肺炎, 急性呼吸窘迫综合征的发生率, 死亡率和需要机械通气的增加显著相关。我们还估计在住院的新型冠状病毒肺炎患者中糖尿病的总体合并患病率为31%。
1 INTRODUCTION
The COVID-19 pandemic is an ongoing public health crisis, with over 245 373 039 confirmed cases globally, including 4 979 421 deaths as of 29 October 2021 (according to the World Health Organization [WHO]).1 Factors associated with poor outcomes, including in-hospital morbidity and mortality, in COVID-19 hospitalized patients are of considerable interest.2 More specifically, health comorbidities may predispose patients to an increased risk of poor outcomes following COVID-19 infection.2-4 Previous studies have indicated a relatively higher prevalence of diabetes in COVID-19 patients compared to those without diabetes.5 Moreover, previous meta-analyses have indicated that diabetes is associated with increased risk of severe COVID-19, acute respiratory distress syndrome (ARDS), and in-hospital mortality.6-11 However, several of these studies included patients under 18 years of age or from the community setting.
It is of clinical and public health interest to understand how diabetes mediates outcomes in COVID-19 hospitalized patients. The current study sought to determine in-hospital prevalence of diabetes in COVID-19 patients and investigate the association of diabetes with COVID-19 severity, ARDS rate, mortality, and the need for mechanical ventilation in hospitalized COVID-19 adult patients by performing a systematic review and meta-analysis.
- What is the pooled prevalence of diabetes in hospitalized COVID-19 patients drawn from the meta-analysis?
- Is diabetes associated with COVID-19 severity, increased rate of ARDS, need for mechanical ventilation, and in-hospital mortality?
2 METHODS
2.1 Literature search: Identification and selection of studies
Relevant articles were retrieved from the following databases until July 2021: PubMed, Embase, and Cochrane Central Register of Controlled Trials. The search terms used included diabetes or diabetic or t1dm or t2dm or diabetes mellitus and covid-19 or covid or coronavirus or severe acute respiratory syndrome coronavirus 2 or SARS-CoV-2. Nonhuman studies and articles not written in English were excluded by applying filters. The detailed search strategy is provided in the Supplementary Information. The Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) flowchart was used to present the search strategy and studies included in the meta-analysis (Figure 1). The PRISMA 2020 (Supplemental Table S6), Meta-analysis of Observational Studies in Epidemiology (MOOSE) (Supplemental Table S5), and Standards for Reporting of Diagnostic Accuracy Studies (STARD 2015) checklists (Supplemental Table S7) were also adhered to for reporting.
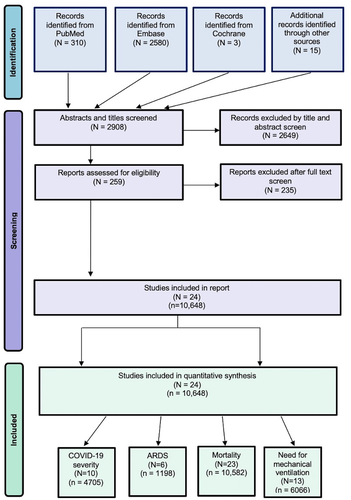
2.2 Inclusion and exclusion criteria
For studies to be included, the following inclusion criteria were applied: (a) age ≥ 18 years, (b) availability of comparative data between diabetes and non-diabetes groups, (c) patients with a confirmed diagnosis of COVID-19 in a hospital setting, and (d) studies with good methodological design (with appropriate sample size deemed to be >20 patients in each group). Besides, the following criteria were applied to exclude studies: (a) nonhuman/animal studies; (b) duplicated publications; (c) nonavailability of full-text articles; (d) case reports, case series, letters, systematic reviews, and meta-analyses; and (e) studies provided in abstract form that did not have relevant data on diabetes or relevant clinical outcomes were not reported.
2.3 Data extraction
The title and abstracts were reviewed on Endnote (X9.3.3; Clarivate) first to rule out that the articles did not meet the eligibility criteria. The remaining articles were examined thoroughly to determine whether they should be included in the systematic review or meta-analysis according to the eligibility criteria. Reference lists of articles included were also reviewed for possible inclusion. The screening was conducted independently by two authors experienced in meta-analysis. Any disagreements were discussed, and final decisions were reached by consensus. The data from each study/trial were extracted independently using a data extraction sheet to obtain the following information: (a) baseline demographics (author, country, and year of publication), (b) study population (age of patients, sample size, characteristics of COVID-19 patients, and presence or absence of diabetes), and (c) outcome measures (severity of COVID-19, in-hospital ARDS, mortality, and need for mechanical ventilation). The outcome measures were tabulated for the diabetes and non-diabetes groups. The definition of severe disease differed between studies, with the presence of respiratory distress or admission to the intensive care unit as common criteria. We dichotomized severity groups into severe and non-severe. Where studies had separate groups for severe and critical cases, these two groups were combined for the purpose of this meta-analysis. ARDS was defined according to the Berlin definition in two studies and undefined in two other studies.12 Mortality was defined as in-hospital death within the study period for all studies. Mechanical ventilation was defined as invasive mechanical ventilation in five studies, intubation in two studies, and ventilation in one study.
2.4 Quality assessment of included studies
The modified Jadad analysis scale was independently used by two researchers to assess the methodological quality of each study.13 The bias due to funding was also evaluated, independent of the quality assessment, based on the declaration of funding sources and conflicts of interest.14
2.5 Statistical analysis
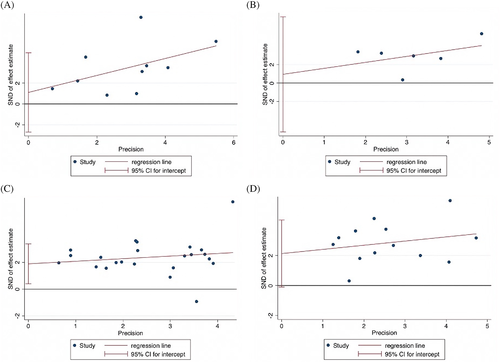
All statistical analyses were performed using STATA (Version 13.0, StataCorp LLC, College Station, Texas). The baseline characteristics of patient populations were synthesized from all included studies. The crude prevalence of diabetes within the overall cohort was determined. Where applicable, median, and interquartile ranges were converted to mean and SD using the method described by Wan et al15 In this study, the association of diabetes with severity of COVID-19, odds of ARDS, mortality, and need for mechanical ventilation was investigated by performing the DerSimonian-Laird random-effects meta-analysis. Summary effects and heterogeneity obtained from the meta-analysis were tabulated. Forest plots were generated to present the odds ratios (OR) (effects measure), 95% CI, percentage weight, and the heterogeneity between studies included in the meta-analysis. When applicable, tests of overall effect, vis a vis P value, and Z-test were also reported. Egger's tests of effect sizes corresponding to each clinical outcome were performed (Figure 2 and Supplemental Table S3). To assess the heterogeneity between the studies, I2 statistics and P values were used (<40% = low, 30%-60% = moderate, 50%-90% = substantial, and 75%-100% = considerable).16 Other heterogeneity parameters including Cochran's Q, H-Test (relative excess in Cochran's Q over its degrees of freedom), and tau (for heterogeneity variance estimates) were also analyzed. The regression-based Egger's test for small-study effects was also used to evaluate funnel plot asymmetry quantitatively (Figure 5). The effects of an individual study on the overall meta-analysis were also evaluated, for stability and sensitivity, using STATA's “metaninf” package (Supplemental Figure S1). Effect size analyses for the association of diabetes with severity, ARDS, mortality and mechanical ventilation are shown in Supplemental Figure S2. A Begg's funnel plot was used to visually detect the presence of publication bias, identified by the presence of asymmetry on the funnel plot (Supplemental Figure S3). P values <.05 indicated statistically significant association.
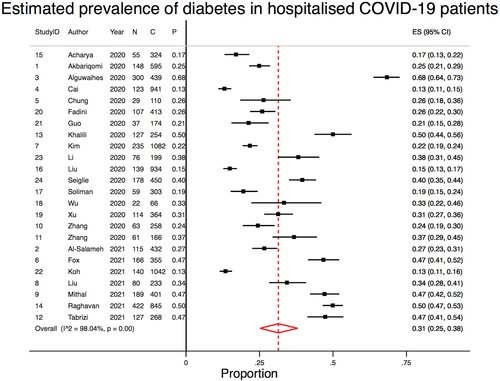
For estimating prevalence, the “metaprop” STATA command was used to pool proportions by performing a DerSimonian-Laird random-effects meta-analysis of proportions obtained from the individual studies.17 To stabilize the variances, Freeman-Tukey double arcsine transformation was also applied to stabilize the variances in order to calculate the pooled estimates. For prevalence meta-analysis, the heterogeneity was estimated from the inverse-variance fixed-effect model as well as by using the I2 measure. Forest plots were created to report the overall estimates of the meta-analysis.
3 RESULTS
3.1 Description of included studies
There were 24 included studies, with a total cohort of 10 648 patients, of whom 3112 had diabetes (29.23%). The mean age ± SD of all included studies was 49.87 ± 32.32 years, and there were 5953 males overall (55.91%). COVID-19 diagnosis was defined as a positive reverse transcription polymerase chain reaction (RT-PCR) test in 21 studies; as history, fever or respiratory symptoms, CT imaging abnormalities, and a positive RT-PCR in 1 study; and was not defined in 2 studies. Three studies specifically investigated type 2 diabetes only, with the remainder not distinguishing between type 1 and 2. Data on diabetes severity or duration were not provided in any studies. Although the overall crude prevalence rate of diabetes was 29.23%, our meta-analysis demonstrated that the overall pooled estimated prevalence rate was 31% (95% CI, 0.25-0.38; z = 16.09, P < .0001). A forest plot showing the prevalence of diabetes in COVID-19 hospitalized patients is included in Figure 3. Supplemental Table S4 shows the full results of the random-effects meta-analysis of proportions obtained from individual studies. Considerable heterogeneity was found between the studies (I2 = 98.04%, P < .0001). A description of the clinical characteristics of the included studies can be found in Table 1. Summary effects and heterogeneity from the meta-analysis on the association of diabetes are provided in Table 2. Supplemental Table S1 provides a summary of significant meta-analysis outcomes. Summary data and performance estimates for sensitivity and specificity analysis are also provided in Supplemental Table S2. The results of methodological quality, risk of bias, and funding bias assessment of included studies are provided in Supplemental Table S3. One study demonstrated a moderate potential for funding bias. Effect size analyses for severe COVID-19, ARDS, mortality, and mechanical ventilation are also presented in Supplemental Figure S2.
| Study ID | Author | Year | Country | Study type | Cohort | Age (mean ± SD) | Male (%) | Severity definition | ARDS definition | Mechanical ventilation definition | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Overall | DM | nDM | Overall | DM | nDM | |||||||||||
| 1 | Akbariqomi28 |
2020 | Iran | Retrospective | 595 | 54.33 ± 13.38 | 53.33 ± 14.97 | 57.3 ± 16.36 | 67.39 | 66.89 | 67.56 | National Health Committee of China criteria | NR | Invasive mechanical ventilation | ||
| 2 | Al-Salameh2 | 2021 | France | Retrospective | 432 | 72.61 ± 15.78 | 72 ± 18.62 | 72.83 ± 14.64 | 55.09 | 52.05 | 63.48 | Berlin definition | ||||
| 3 | Alguwaihes32 | 2020 | Saudi Arabia | Retrospective | 439 | 55.2 ± 13.74 | NR | NR | 68.34 | 66.67 | 71.94 | Required intubation | ||||
| 4 | Cai33 |
2020 | China | Retrospective | 941 | 57.02 ± 12.46 | 68.41 ± 14 | 56 ± 12.15 | 48.25 | 49.59 | 48.04 | NR | Invasive mechanical ventilation | |||
| 5 | Chung36 |
2020 | South Korea | Retrospective | 110 | 56.9 ± 17 | 66.3 ± 8.9 | 53.5 ± 17.9 | 43.64 | 48.28 | 41.98 | Chinese Center for Disease Control and Prevention criteria | Berlin definition | Invasive mechanical ventilation | ||
| 6 | Fox34 | 2021 | USA | Retrospective | 355 | 66.21 ± 14.21 | 66.42 ± 12.67 | 66.03 ± 15.46 | 49.01 | 51.81 | 46.56 | Need for intubation | ||||
| 7 | Kim39 | 2020 | South Korea | Retrospective | 1082 | 56.06 ± 17.55 | 68.3 ± 11.9 | 56.5 ± 18 | 35.49 | 45.11 | 32.82 | Severe disease defined as at least one of: ICU care, high-flow O2 nasal cannulae, mechanical ventilation, CRRT, or ECMO | Mechanical ventilation | |||
| 8 | Liu31 | 2021 | China | Retrospective | 233 | 62.33 ± 14.17 | 65.33 ± 10.7 | 63.5 ± 19.09 | 49.36 | 51.25 | 48.37 | National Health Committee of China criteria | ||||
| 9 | Mithal35 | 2021 | India | Prospective | 401 | 54.06 ± 12.35 | 59.8 ± 12.1 | 47.7 ± 16.5 | 68.83 | 74.6 | 63.68 | WHO Ordinal Scale 5 and above | ||||
| 10 | Zhang40 | 2020 | China | Retrospective | 258 | 63.33 ± 10.44 | 64.33 ± 10.62 | 63 ± 11.2 | 53.49 | 60.32 | 51.28 | National Health Committee of China criteria | Berlin definition | Invasive mechanical ventilation | ||
| 11 | Zhang38 | 2020 | China | Retrospective | 166 | 62.7 ± 14.2 | 65.6 ± 11.4 | 61.04 ± 15.34 | 51.2 | 54.1 | 49.52 | National Health Committee of China Criteria | Invasive mechanical ventilation | |||
| 12 | Tabrizi41 | 2021 | Iran | Retrospective | 268 | 57.33 ± 17.14 | 63.67 ± 12.75 | 50 ± 17.23 | 53.36 | 53.54 | 53.19 | Invasive mechanical ventilation | ||||
| 13 | Khalili42 | 2020 | Iran | Retrospective | 254 | 65.7 ± 12.51 | 66.28 ± 12.51 | 65.03 ± 12.53 | 55.91 | 55.91 | 55.91 | Berlin definition | Invasive mechanical ventilation | |||
| 14 | Raghavan43 | 2021 | India | Retrospective | 845 | 55.51 ± 15.78 | 51 ± 17 | 60 ± 13 | 65.44 | 67.54 | 63.36 | Need for intubation | ||||
| 15 | Acharya37 | 2020 | South Korea | Retrospective | 324 | 55 ± 21.4 | 69.8 ± 13.5 | 51.9 ± 21.4 | 41.67 | 36.36 | 42.75 | |||||
| 16 | Liu44 | 2020 | China | Retrospective | 934 | 13.96 ± 62.03 | 64.5 ± 10 | 61.6 ± 14.5 | 48.61 | 47.48 | 48.81 | NR | ||||
| 17 | Soliman45 | 2020 | Qatar | Retrospective | 303 | 13.25 ± 39.31 | 52.1 ± 12.67 | 36.22 ± 11.43 | NR | NR | Mechanical ventilation | |||||
| 18 | Wu46 | 2020 | China | Retrospective | 66 | 14.71 ± 49.5 | 52.55 ± 13.7 | 47.98 ± 15.11 | 66.67 | 72.73 | 63.64 | National Health Committee of China Criteria | ||||
| 19 | Xu47 | 2020 | China | Retrospective | 364 | 64.33 ± 13.4 | 65.33 ± 12.01 | 63 ± 15.66 | 56.59 | 54.39 | 57.6 | |||||
| 20 | Fadini48 | 2020 | Italy | Retrospective | 413 | 64.9 ± 15.4 | 69.7 ± 13.8 | 63.3 ± 15.5 | 59.32 | 65.42 | 57.19 | Composite of admission to the ICU (including all subjects needing mechanical ventilation) or death | ||||
| 21 | Guo49 | 2020 | China | Retrospective | 174 | 58.33 ± 13.46 | 61.67 ± 10.8 | 57 ± 14.24 | 43.68 | 54.05 | 40.88 | |||||
| 22 | Koh50 | 2021 | Singapore | Retrospective | 1042 | 39 ± 11 | 48 ± 13 | 36.82 ± 10.19 | 95.39 | 92.14 | 95.9 | WHO criteria | ||||
| 23 | Li51 | 2020 | China | Retrospective | 199 | 62.67 ± 18.67 | 68.67 ± 10.8 | 57 ± 14.24 | 44.72 | 65.79 | 31.71 | |||||
| 24 | Seiglie52 | 2020 | USA | Retrospective | 450 | 17.29 ± 63.62 | 66.7 ± 14.2 | 61.6 ± 18.8 | 57.56 | 61.8 | 54.78 | |||||
| Study ID | Smoking (current or past), n (%) | Obesity, n (%) | Hypertension, n (%) | CVD, n (%) | Pulmonary disease, n (%) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Overall | DM | nDM | Overall | DM | nDM | Overall | DM | nDM | Overall | DM | nDM | Overall | DM | nDM | ||
| 1 | 40 (6.7) | 9 (6) | 31 (6.9) | 176 (29.6) | 48 (32.4) | 128 (28.6) | 172 (28.9) | 72 (48.6) | 100 (22.3) | 112 (18.8) | 40 (27) | 72 (16.1) | 87 (14.6) | 24 (16.2) | 63 (14.09) | |
| 2 | 105 (35.84) | 28 (35.4) | 77 (36.0) | 124 (37.7) | 37 (32.2) | 87 (27.4) | 255 (59.2) | 91 (79.1) | 164 (51.7) | 148 (34.3) | 49 (42.6) | 99 (31.2) | 39 (9.0) | 6 (5.2) | 33 (10.4) | |
| 3 | 9 (2.6) | 178 (42.2) | 187 (42.6) | 44 (10.0) | ||||||||||||
| 4 | 272 (28.9) | 66 (53.7) | 206 (25.2) | 35 (3.7) | 6 (4.9) | 29 (3.5) | ||||||||||
| 5 | 16 (14.5) | 7 (24.1) | 9 (11.) | 37 (33.6) | 16 (55.2) | 21 (25.9) | 10 (9.1) | 5 (17.2) | 5 (6.2) | 4 (3.6) | 2 (6.9) | 2 (2.5) | ||||
| 6 | 272 (76.6) | 151 (90.9) | 121 (64.0) | 45 (12.7) | 22 (13.3) | 23 (12.2) | ||||||||||
| 7 | 374 (34.6) | 147 (62.6) | 227 (26.8) | 72 (6.7) | 16 (6.8) | 56 (6.6) | ||||||||||
| 8 | 90 (38.6) | 43 (53.8) | 47 (30.7) | 20 (8.6) | 8 (10.0) | 12 (7.8) | ||||||||||
| 9 | 164 (40.9) | 111 (58.7) | 53 (25.0) | 24 (6.0) | 10 (5.3) | 14 (6.6) | ||||||||||
| 10 | 98 (38.0) | 29 (46.0) | 69 (35.4) | 39 (15.1) | 15 (23.8) | 24 (12.3) | 9 (3.5) | 2 (3.2) | 7 (3.6) | |||||||
| 11 | 31 (18.7) | 12 (19.7) | 19 (18.1) | 91 (54.8) | 37 (60.7) | 54 (51.4) | 76 (45.8) | 35 (56.4) | 41 (39.0) | 30 (18.1) | 16 (26.2) | 14 (13.3) | 19 (11.4) | 9 (14.7) | 10 (9.5) | |
| 12 | 85 (32.7) | 63 (50.8) | 22 (16.2) | 110 (41.0) | 75 (59.5) | 35 (25.0) | 27 (10.0) | 14 (11.0) | 13 (9.3) | |||||||
| 13 | 14 (5.5) | 8 (6.3) | 6 (4.7) | 109 (42.9) | 68 (53.5) | 41 (32.3) | 7 (2.8) | 4 (3.1) | 3 (2.4) | |||||||
| 14 | 352 (41.9) | 247 (58.4) | 105 (24.9) | |||||||||||||
| 15 | 55 (17.0) | 11 (20.0) | 44 (16.4) | 80 (24.7) | 32 (58.2) | 48 (17.8) | 19 (5.9) | 8 (14.6) | 11 (4.1) | |||||||
| 16 | ||||||||||||||||
| 17 | 46 (15.2) | 31 (52.5) | 15 (6.1) | |||||||||||||
| 18 | 27 (40.9) | 12 (44.4) | 15 (55.6) | |||||||||||||
| 19 | ||||||||||||||||
| 20 | 53 (27.7) | 15 (28.3) | 38 (27.5) | 212 (51.3) | 73 (68.2) | 139 (45.4) | 72 (18.0) | 27 (26.0) | 45 (15.3) | |||||||
| 21 | 43 (24.7) | 10 (27.0) | 33 (24.1) | 32 (18.4) | 12 (32.4) | 20 (14.6) | 14 (9.7) | 2 (5.4) | 12 (8.7) | |||||||
| 22 | ||||||||||||||||
| 23 | ||||||||||||||||
| 24 | 191 (42.4) | 91 (51.4) | 100 (36.8) | 178 (39.6) | 134 (75.3) | 44 (24.7) | 110 (24.4) | 46 (25.8) | 66 (24.3) | |||||||
| Study ID | Severity, n (%) | ARDS, n (%) | Mortality, n (%) | Mechanical ventilation, n (%) | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| DM severe | nDM severe | DM | nDM | DM | nDM | DM | nDM | |||||||||
| 1 | 36 (24.32) | 55 (12.3) | 26 (17.57) | 39 (8.72) | 16 (10.81) | 12 (2.68) | ||||||||||
| 2 | 31 (26.96) | 49 (15.51) | 20 (17.39) | 68 (21.45) | ||||||||||||
| 3 | 60 (20.48) | 17 (9.29) | 60 (20.27) | 17 (12.32) | ||||||||||||
| 4 | 47 (38.21) | 138 (16.87) | 21 (17.07) | 76 (9.29) | 11 (8.94) | 29 (3.55) | ||||||||||
| 5 | 10 (43.48) | 68 (91.89) | 11 (37.93) | 7 (8.64) | 5 (17.24) | 1 (1.23) | 8 (27.59) | 3 (3.7) | ||||||||
| 6 | 45 (27.11) | 35 (18.52) | 48 (28.92) | 41 (21.69) | ||||||||||||
| 7 | 170 (18.78) | 65 (40.88) | 44 (18.72) | 41 (4.84) | 37 (15.74) | 38 (4.49) | ||||||||||
| 8 | 26 (32.5) | 89 (58.17) | 18 (22.5) | 9 (5.88) | ||||||||||||
| 9 | 151 (79.89) | 193 (91.04) | 12 (6.35) | 3 (1.42) | ||||||||||||
| 10 | 18 (28.57) | 69 (35.38) | 24 (38.10) | 38 (19.49) | 7 (11.11) | 8 (4.1) | 7 (11.11) | 9 (4.62) | ||||||||
| 11 | 9 (14.75) | 21 (20) | 13 (21.31) | 11 (10.48) | 9 (14.75) | 2 (1.9) | ||||||||||
| 12 | 22 (17.32) | 8 (5.67) | 23 (18.11) | 4 (2.84) | ||||||||||||
| 13 | 21 (16.54) | 19 (14.96) | 29 (22.83) | 19 (14.96) | 19 (14.96) | 8 (6.3) | ||||||||||
| 14 | 43 (10.19) | 25 (5.91) | 6 (1.42) | 5 (1.18) | ||||||||||||
| 15 | 11 (20) | 13 (4.83) | ||||||||||||||
| 16 | 139 (100) | 773 (97.23) | 4 (2.88) | 9 (1.13) | ||||||||||||
| 17 | 14 (23.73) | 10 (4.1) | ||||||||||||||
| 18 | 7 (31.82) | 4 (9.09) | ||||||||||||||
| 19 | 27 (23.68) | 32 (12.8) | ||||||||||||||
| 20 | 40 (37.38) | 62 (20.26) | 15 (14.02) | 33 (10.78) | ||||||||||||
| 21 | 4 (10.81) | 5 (3.65) | ||||||||||||||
| 22 | 31 (22.14) | 20 (2.22) | 4 (2.86) | 1 (0.11) | ||||||||||||
| 23 | 11 (14.47) | 7 (3.14) | ||||||||||||||
| 24 | 28 (15.73) | 22 (8.09) | 66 (37.08) | 63 (23.16) | ||||||||||||
- Abbreviations: ARDS, acute respiratory distress syndrome; CRRT, continuous renal replacement therapy; CVD, cardiovascular disease; DM, diabetes mellitus; ECMO, extracorporeal membrane oxygenation; ICU, intensive care unit; nDM, no diabetes mellitus; NR, not reported; WHO, World Health Organization.
| Outcome | Summary effects | |||||||
|---|---|---|---|---|---|---|---|---|
| REDL | Heterogeneitya | Heterogeneity variance estimates | ||||||
| Effect measure | OR (95% CI) | Tests of overall effect | Cochran's Q | H | I2b | P value | tau≤c | |
| COVID-19 severity | OR | 3.39 (2.14-5.37) | P < .0001, z = 5.206 | 40.21 | 2.11 (95% CI, 1.48-2.71) | 77.6% (95% CI, 54.2%-86.4%) | P < .0001 | 0.3706 |
| ARDS | OR | 2.55 (1.74-3.75) | P < .0001, z = 4.772 | 11.05 | 1.49 (95% CI, 1.00-2.42) | 54.7% (95% CI, 0%-79.9%) | P = .05 | 0.1200 |
| Mortality | OR | 2.44 (1.93-3.09) | P < .0001, z = 7.425 | 48.47 | 1.48 (95% CI, 1.111-1.845) | 54.6% (95% CI, 19%-70.6%) | P = .001 | 0.1586 |
| Need for mechanical ventilation | OR | 3.03 (2.17-4.22) | P < .0001, z = 6.524 | 29.93 | 1.58 (95% CI, 1.06-2.07) | 59.9% (95% CI, 11.3%-76.7%) | P = .003 | 0.1974 |
- Abbreviations: ARDS, acute respiratory distress syndrome; H, relative excess in Cochran's Q over its degrees of freedom; I2, proportion of total variation in effect estimate due to between-study heterogeneity (based on Cochran Q); OR, odds ratio; Q, heterogeneity measures were calculated from the data with CI based on noncentral chi-square (common effect) distribution for Cochran Q test; REDL, DerSimonian-Laird random-effects method.
- a Heterogeneity measures were calculated from the data with 95% CI based on gamma (random effects) distribution for Q.
- b Values of l2 are percentages.
- c Heterogeneity variance estimates (tau≤) were derived from REDL.
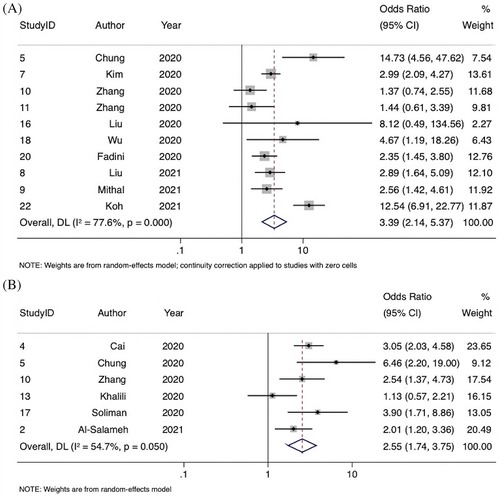
3.2 Association of diabetes with severe COVID-19
Overall, 10 studies were included in the meta-analysis of the association of diabetes with severe COVID-19, comprising 4705 patients. Severity of disease definitions varied between studies and included criteria such as admission to the intensive care unit, oxygen stats, and need for intubation. Diabetes was associated with significantly increased odds of severe COVID-19 (OR 3.39; 95% CI, 2.14-5.37; P < .0001, z = 5.206) (Figure 4 and Table 2). Substantial heterogeneity was found between the studies (I2 = 77.6% [95% CI, 2.7%-90.4%], P < .0001). There was some evidence of publication bias from visualization of the funnel plot (Supplemental Figure S3).
3.3 Association of diabetes with ARDS
Six studies were included in the meta-analysis of the association of diabetes with in-hospital ARDS, comprising 2298 patients. ARDS was defined by the Berlin definition in four studies and undefined in two. Diabetes was associated with significantly increased odds of ARDS (OR 2.55; 95% CI, 1.74-3.75; P < .0001, z = 4.772) (Figure 4). Moderate-to-substantial heterogeneity was found between the studies (I2 = 54.7% [95% CI, 0%-82.9%], P = .05). There was some evidence of publication bias observed by visual inspection of the funnel plot (Supplemental Figure S3).
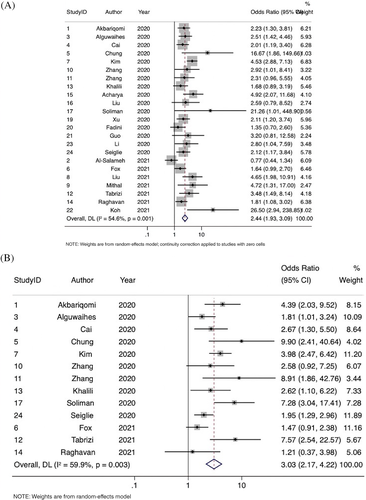
3.4 Association of diabetes with in-hospital mortality
Overall, 23 studies were included in the meta-analysis of the association of diabetes with mortality, comprising 10 582 patients. Mortality was defined as the death of a patient within the follow-up period of the study in all included studies. Diabetes was significantly associated with increased odds of in-hospital mortality (OR 2.44; 95% CI, 1.93-3.09; P < .0001, z = 7.425) (Figure 5). Moderate-to-substantial heterogeneity was found between the studies (I2 = 54.6% [95% CI, 3.8%-73.7%], P = .001). No evidence of publication bias was observed by visual inspection of the funnel plot (Supplemental Figure S3).
3.5 Association of diabetes with the need for mechanical ventilation
Overall, 13 studies were included in the meta-analysis of the association of diabetes with the requirement of mechanical ventilation, comprising 6066 patients. Mechanical ventilation was defined as invasive mechanical ventilation in seven studies, need for intubation in two studies, and mechanical ventilation in three studies. Diabetes was associated with significantly increased odds of need of mechanical ventilation (OR 3.03; 95% CI, 2.17-4.22; P < .0001, z = 6.524) (Figure 5). Moderate-to-substantial heterogeneity was found between the studies (I2 = 59.9% [95% CI, 0%-80.5%], P = .003). There was some evidence of publication bias observed by visual inspection of the funnel plot (Supplemental Figure S3).
4 DISCUSSION
Our study clearly demonstrates that diabetes in COVID-19 hospitalizedpatients is associated with poor clinical outcomes. Diabetes was significantly associated with increased odds of severe COVID-19, need for mechanical ventilation, ARDS, and in-hospital mortality. This is consistent with previous studies investigating the association of diabetes with certain clinical outcomes; however, several key clinical endpoints were not reported.6-11 Therefore, our study provides evidence on how diabetes mediates outcomes in hospitalized COVID-19 adult patients. The crude prevalence of diabetes in hospitalized patients varied from 15% to 40% in various studies.18-20 Our meta-analysis estimated an overall pooled prevalence of 31% of diabetes in hospitalized COVID-19 patients.
Various mechanisms have been implicated in the poor clinical trajectory due to COVID-19 in diabetes patients. Diabetes-induced hyperglycemia leads to several issues, including chronic inflammation and impairment of the immune system through oxidative stress and diminished functioning of antibodies, macrophages, and chemokines.21, 22 It is known that COVID-19 further exacerbates inflammatory responses, potentially resulting in cytokine storms.22 It also contributes to diabetes-related issues such as endothelial dysfunction and coagulation-related issues.23 It has also been postulated that diabetes-related alveolar microangiopathy in the lungs could be contributing to worsened clinical outcomes.24 These complications may lead to the increased severity, acute respiratory distress, and mortality seen in diabetes patients.25
Several factors may contribute to the clinical outcomes of COVID-19 in patients with diabetes.26, 27 There is a close relationship between diabetes and cardiovascular complications such as obesity and hypertension.28-31 After controlling for these conditions and other comorbidities, some studies included in this meta-analysis found that there was no significant association between diabetes and mortality from COVID-19.2, 32-34 Hypertension itself is an important risk factor within COVID-19 patients leading to worsened outcome.35 Other important risk factors include disease duration, age, and fasting blood glucose (FBG).28, 36, 37 Cai et al33 found a significant relationship between higher FBG levels and mortality but not between diabetes and mortality. Similarly, Zhang et al38 found a significant association between higher FBG and poor clinical outcomes. This highlights the importance of glucose testing of COVID-19 patients, and not only relying on previous history of diabetes. Given the known severity of COVID-19 in elderly patients, age should also be closely considered. In a retrospective study, Kim et al39 found that there was a significant association between diabetes and mortality in older COVID-19 patients, but not in younger.
There are several limitations for this meta-analysis. Out of the included studies, only Mithal et al35 was prospective in design. This means that the criteria for inclusion in the diabetes group relied largely on previous clinical history and would have excluded some new diabetes cases. Consequently, there may be some patients with undiagnosed diabetes included in the control group. The data on body mass index, diabetes duration, and glycosylated hemoglobin levels are not available for all studies to allow a meta-analysis to be performed. Detailed information on the diabetes profile, such as its duration, have not been reported. The effect of these factors, including impact of poor glycemic control, on COVID-19 severity and outcomes in COVID-19 patients with diabetes are subject of future investigation. Another major limitation is the variation in outcome definitions. In particular, the outcomes of severity and need for mechanical ventilation had varied definitions (Table 1). Findings should be interpreted on methodological design and the study population. However, given that we performed a random-effects model, some of these variabilities and heterogeneities will be covered. Future studies on long-term impact of COVID-19 on patients with diabetes would provide insights on the optimal management strategies.
In conclusion, diabetes is an important clinical consideration in the current COVID-19 pandemic. Our meta-analysis clearly demonstrates that diabetes is associated with poor outcomes such as severe disease, need for mechanical ventilation, ARDS, and mortality. This has implications for the importance of tailored strategies for management of COVID-19 patients with diabetes.
ACKNOWLEDGEMENTS
Funding for the NSW Brain Clot Bank (Chief Investigator: Dr Bhaskar) from the NSW Ministry of Health (2019-2022) is acknowledged. The funding body has no role in the study design, data collection, analysis, interpretation of findings, and manuscript preparation. The content is solely the responsibility of the authors and does not necessarily represent the official views of the affiliated/funding organization/s.
CONFLICT OF INTEREST
The authors declare that they have no conflict of interest.
AUTHOR CONTRIBUTIONS
Sonu M. M. Bhaskar conceived the study; contributed to the planning, methodology, draft, and revision of the manuscript; and supervised the students. Sonu M. M. Bhaskar encouraged Sian A. Bradley to investigate and supervised the findings of this work. Sian A. Bradley and Sonu M. M. Bhaskar wrote the first draft of this paper, and Sian A. Bradley was involved in the investigation, data collection, data curation, and analysis. All authors contributed to the writing and revision of the manuscript. All authors approved the final draft of the manuscript.
AVAILABILITY OF DATA AND MATERIALS
The original contributions presented in the study are included in the article and online Supplementary Information. Further inquiries can be directed to the corresponding author.




